|
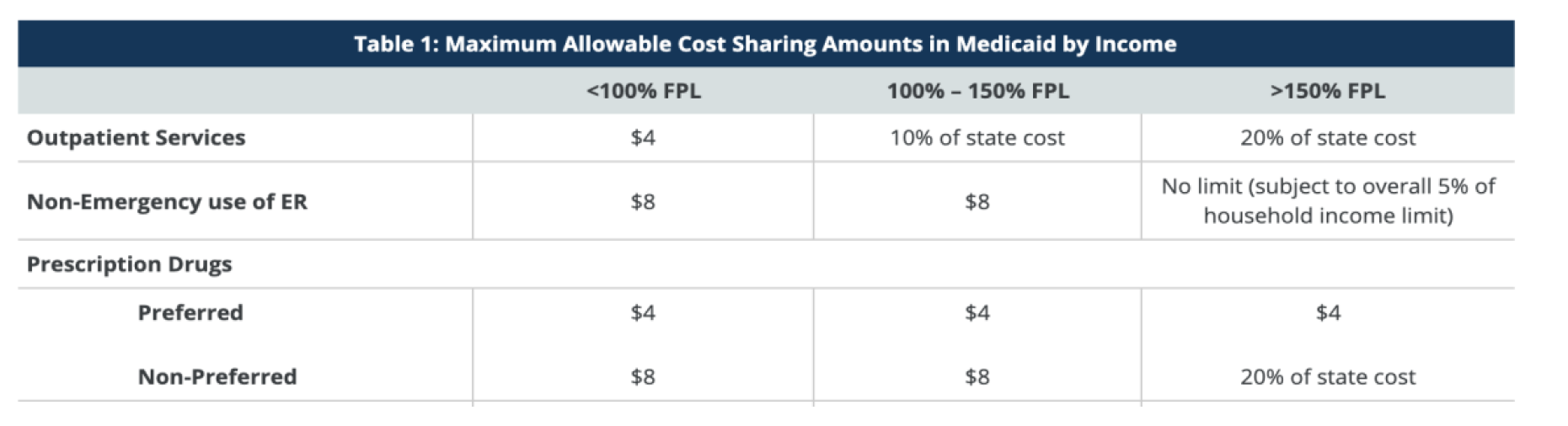
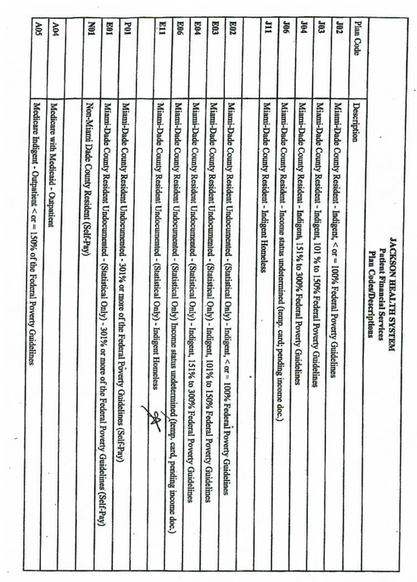
Background and import of JHS: Jackson Health System (JHS) is a vitally important, publicly funded health system serving the Miami-Dade community.[1] For over 100 years, Jackson Memorial Hospital has served as the major source of care for the county’s large uninsured, low-income population.[2] Jackson’s COVID-era policies aimed at addressing health disparities and increasing access to critical healthcare have served as a model for the rest of the state. Jackson’s early willingness to accept self-attestation of a medical condition, to demonstrate vaccination eligibility, was an important break from state policy,[3] and a recognition of the need to innovative service approaches. Jackson’s charity care program and co-payment charges Uninsured county residents are eligible for the Jackson Prime Financial Assistance Program, which entitles county residents to free or reduced-cost care at JHS, based on a sliding income scale.[4] Information on applying can be found here. County residents who are eligible for the Jackson Prime Program are assigned a classification based on income, and given a “J code” (see “PlanCode Description”, Attachment A)[5]. An individual with an income of less than 100% of the federal poverty level (FPL) ($1,073/month or $12,880/year), for example, receives a J02 code.[6] The J “code” determines the fees charged for different types of services. Those charges can be found on the Financial Assistance page of Jackson’s website here. The costs for outpatient services for someone with a J02 code include, e.g., specialty care ($40), procedures ($100), radiology ($15). Even minimal cost sharing results in reduced use of medically necessary care and/or causes families to cut back on other necessities. A significant amount of research over the last forty years has shown that charging low-income individuals even small co-payments worsens their health outcomes. When presented with co-payments that exceed the household budget, low-income people will either forgo needed health care or forgo other basic needs such as food, rent, or phone service, in order to pay for care. This burden not only adversely affects the individual’s health outcomes, it also places financial strain on indigent families who are already struggling to pay for housing, food, transportation, and phone service.[7] Consistent with this undisputed research, the Medicaid program requires that cost sharing for low-income individuals must be de minimis, e.g., no more than $4 for any outpatient service for someone below the poverty line. Table 1 below shows the Medicaid cost sharing limits.[8] Jackson’s charges are too high. JHS’s charge for an indigent patient needing to see a specialist ($40) is 10 time Medicaid’s $4.00 maximum charge. Jackson’s charge for an outpatient procedure ($100) is 25 times that which Medicaid allows. Consider the hypothetical (but all too real) case of an individual whose monthly income is less than $1,073, and who is experiencing intestinal bleeding. This person will likely need to be seen first by a gastroenterologist, at a cost of $40, and will then likely need a procedure, such as a colonoscopy, to diagnose the cause of the bleeding, costing an additional $100. Someone with little or no income will simply not be able to pay these charges. As a result, they will likely forego the needed care until the situation becomes urgent, at which point they will seek treatment in the emergency room. Should the patient learn they have colon cancer, every visit with the oncologist will cost $40, every radiation treatment will cost $15. These costs too are out of reach, forcing the individual and/or their family members to make impossible choices. Conclusion: JHS’ current copayment charges exponentially exceed appropriate cost sharing limits, as determined by decades of research, and adopted by the Medicaid program. In order for JHS to fully align its policies and practices with its mission and history, and to best serve Miami-Dade County’s approximately 500,000 uninsured residents living below the poverty line,[9] copayment charges must be revised consistent with well-established research and the maximum cost sharing allowed under the Medicaid program. Download PDF
Prepared by Miriam Harmatz, Advocacy Director & Founder, Florida Health Justice Project (FHJP) and Maya Rosen, FHJP Intern, Harvard Class of 2025. For questions contact [email protected]. June 2021.
Attachment A ____________________________________________________________ [1] Jackson Health, “About Jackson Health System,” available at https://jacksonhealth.org/about-us/ [2] Jackson Health, “Our History,” available athttps://jacksonhealth.org/about-us/#our-history [3] Prior to Jackson’s adoption of self-attestation, and pursuant to state policy, uninsured county residents were required to produce a physician's note deeming them “medically vulnerable.” This state policy created an obvious barrier as Florida remains one of 12 states that has refused to expand Medicaid. As a result of this refusal, most low-income uninsured adults do not have a personal physician and thus could not produce the requisite note. [4] Jackson Health, “Financial Assistance,” available at https://jacksonhealth.org/patient-tools/financialassistance/ Note, this link goes to the JHS web site landing page entitled “Financial Assistance.” Relevant forms regarding the program are at the bottom of the landing page under downloadable forms. These include: “Financial Assistance Application,” “Jackson Health Fee Systems,” and “Third Party Verification Statement.” Note: the Jackson Prime Financial Assistance Program Summary, also found at the bottom of the landing page, describes the process for applying. The documents which are required may prove to be barriers for undocumented county residents who wish to apply for the program, e.g. proof of immigration status, social security card. [5] The JHS website does not appear to have a document describing which J code applies based on income. A copy of the J code designations based on income is at Attachment A. [6] 2021 Federal Poverty Guidelines, available at https://aspe.hhs.gov/2021-poverty-guidelines [7] Leighton Ku & Victoria Wachino, Center on Budget & Policy Priorities, The Effect of Increased Cost- Sharing in Medicaid: A Summary of Research Findings (2005), https://www.cbpp.org/archiveSite/5-31- 05health2.pdf ; see also Henry J. Kaiser Family Foundation, “The Effects of Premiums and Cost Sharing on Low-Income Populations: Updated Review of Research Findings”, June 1, 2017, available at: https://www.kff.org/medicaid/issue-brief/the-effects-of-premiums-and-cost-sharing-on-low-incomepopulations-updated-review-of-research-findings/ [8] Source: Table 1, Page 3 of Henry J. Kaiser Family Foundation, “The Effects of Premiums and Cost Sharing on Low-Income Populations: Updated Review of Research Findings”, June 1, 2017, available at: https://www.kff.org/medicaid/issue-brief/the-effects-of-premiums-and-cost-sharing-on-low-income-populationsupdated-review-of-research-findings/ [9] United States Census Bureau Data, available at https://www.census.gov/quickfacts/fact/table/miamidadecountyflorida/POP060210 According to the census, approximately 20% of Miami-Dade County residents under 65 years of age are uninsured. Given that 83.3% of the 2,716,940 residents of MDC are under 65, this quantifies to about 500,000 residents. Comments are closed.
|
Sign-up For Email Updates |
The Florida Health Justice Project, a nonprofit organization, recognizes that access to quality and affordable health care is a human right and engages in comprehensive advocacy to expand healthcare access and promote health equity for vulnerable Floridians.
A COPY OF THE OFFICIAL REGISTRATION AND FINANCIAL INFORMATION MAY BE OBTAINED FROM THE DIVISION OF CONSUMER SERVICES BY CALLING TOLL FREE WITHIN THE STATE AT 1-800-435-7352 . IT CAN ALSO BE FOUND AT WWW.800HELPFLA.COM. REGISTRATION DOES NOT IMPLY ENDORSEMENT, APPROVAL OR RECOMMENDATIONS BY THE STATE.
|